The Evolution of Personal Health Monitoring
The first generation of health wearables told us how many steps we took. The second generation told us our heart rate. The third generation added single-lead ECG and blood oxygen monitoring. But these individual metrics, viewed in isolation, offer limited insight into the complex, dynamic system that is human physiology.
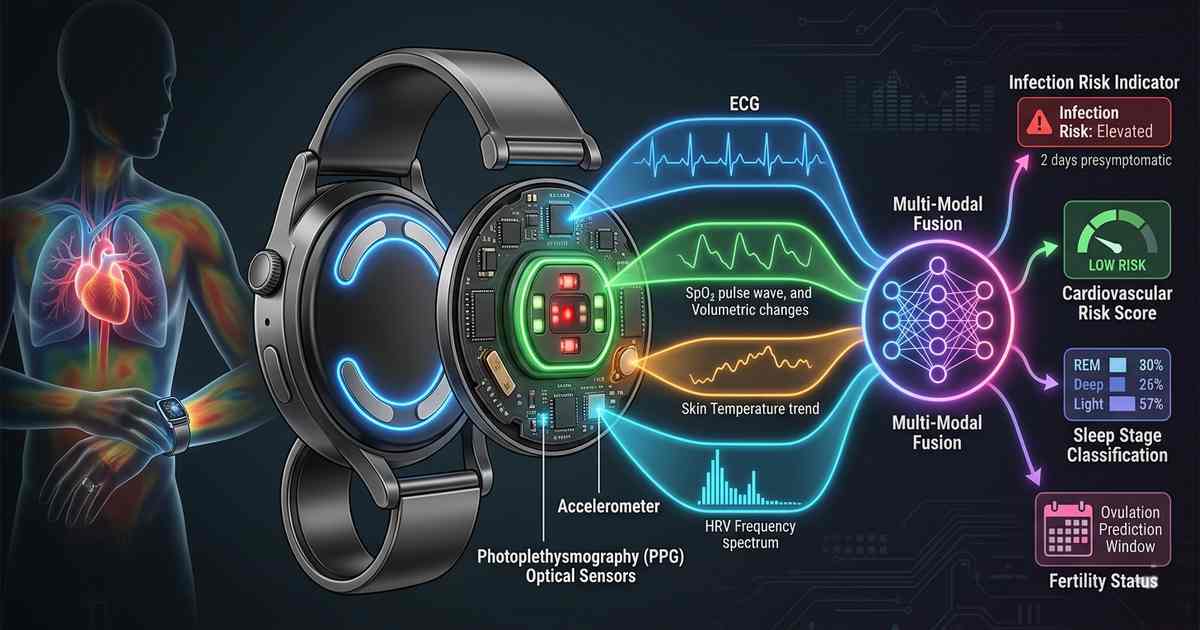
We are now entering the fourth generation of health wearables: multi-modal systems that continuously integrate multiple physiological signals—electrocardiogram (ECG), peripheral capillary oxygen saturation (SpO₂), skin temperature, heart rate variability (HRV), and more—into unified models of individual health. These systems don’t just track metrics; they learn what “normal” means for each user and detect deviations that may signal emerging illness, chronic disease progression, or recovery status.
The promise is transformative: wearables that predict respiratory infections before symptoms appear, detect atrial fibrillation with unprecedented accuracy, monitor cardiovascular recovery, and provide early warnings of developing conditions like hypertension, diabetes, or sleep disorders. This article explores the sensor technologies, data integration challenges, predictive algorithms, and clinical validation of multi-modal health wearables.
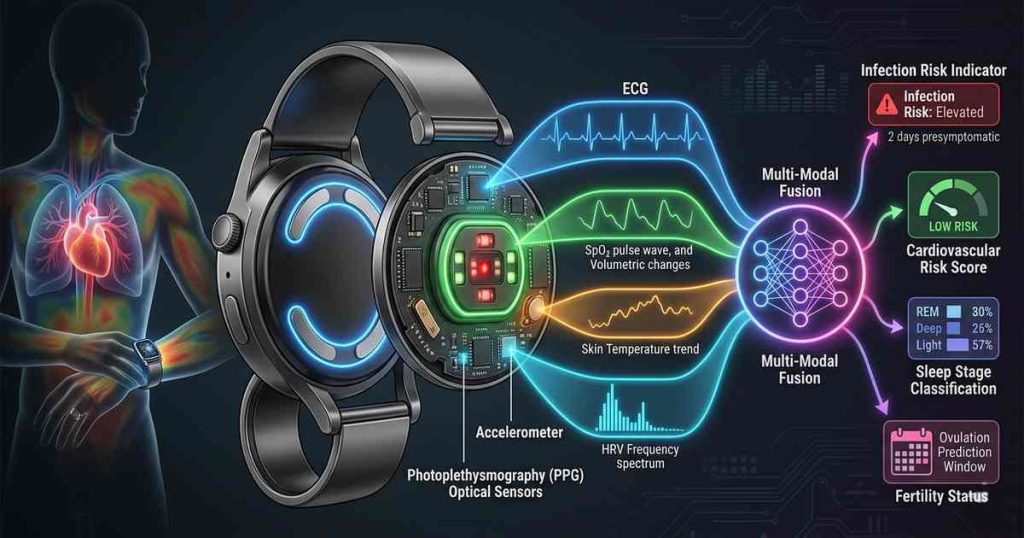
The Sensor Modalities: What They Measure and Why
Electrocardiogram (ECG)
The ECG captures the electrical activity of the heart, providing detailed information about cardiac rhythm, rate, and morphology. In multi-modal wearables, ECG typically uses a single-lead configuration—two electrodes contacting the skin (often at the wrist and finger or wrist and chest).
What ECG provides:
- Heart rate and rhythm classification (sinus, atrial fibrillation, tachycardia, bradycardia)
- QRS complex morphology (potential indicators of ventricular abnormalities)
- PR interval (atrioventricular conduction)
- QT interval (ventricular repolarization, relevant for medication safety)
Clinical applications: Atrial fibrillation detection remains the most validated use case. The Apple Heart Study, with over 400,000 participants, demonstrated that wrist-based ECG could identify AF with high positive predictive value when followed by confirmatory patch monitoring. Beyond AF, ECG-based QTc monitoring is emerging for patients taking medications that prolong QT interval (certain antidepressants, antibiotics, antiarrhythmics).
Peripheral Capillary Oxygen Saturation (SpO₂)
SpO₂ measures the percentage of hemoglobin saturated with oxygen. Pulse oximetry uses light absorption at two wavelengths (red and infrared) to differentiate oxygenated from deoxygenated blood.
What SpO₂ provides:
- Baseline oxygen saturation (typically 95-100%)
- Overnight desaturation events (potential sleep apnea indicator)
- Decline during respiratory illness (COVID-19, pneumonia, COPD exacerbation)
- Exercise oxygen response (cardiopulmonary fitness)
Clinical applications: The COVID-19 pandemic accelerated SpO₂ integration into consumer wearables. “Silent hypoxia”—dangerously low oxygen without perceived breathlessness—became a recognized phenomenon, and wearables offered continuous monitoring that could prompt earlier medical intervention. For sleep apnea screening, overnight SpO₂ tracking can identify desaturation patterns that warrant formal sleep study.
Skin Temperature
Continuous skin temperature monitoring, typically at the wrist, provides insight into thermoregulation and circadian rhythms. Unlike single-time-point temperature measurements, continuous monitoring reveals patterns and deviations.
What skin temperature provides:
- Circadian rhythm phase (temperature minimum typically occurs 2-4 hours before waking)
- Fever detection (elevation above baseline)
- Ovulation timing (temperature rise after ovulation in menstruating individuals)
- Inflammatory responses (subtle temperature elevations)
- Recovery status (elevated temperature during illness, return to baseline with recovery)
Clinical applications: Fertility tracking is the most established use—skin temperature reliably identifies the post-ovulatory temperature rise, enabling ovulation prediction and menstrual cycle phase detection. Fever detection during illness provides objective evidence of systemic inflammation. Emerging research links sustained nighttime temperature elevation with inflammation and chronic disease activity.
Heart Rate Variability (HRV)
HRV measures the variation in time between successive heartbeats. While heart rate tells you how fast the heart is beating, HRV reveals the balance between the sympathetic (fight-or-flight) and parasympathetic (rest-and-digest) nervous systems.
What HRV provides:
- Autonomic nervous system balance
- Stress and recovery status
- Sleep quality assessment
- Cardiovascular fitness
- Infection detection (HRV typically drops before symptom onset)
Clinical applications: HRV has emerged as perhaps the most sensitive early indicator of physiological stress. Research during the COVID-19 pandemic showed that HRV declines days before symptom onset, enabling presymptomatic infection detection. For athletes, HRV guides training load—low HRV suggests inadequate recovery and increased injury risk. In mental health, HRV correlates with anxiety and depression severity and may track treatment response.
The Power of Multi-Modal Integration
Individual sensors provide valuable data, but the true power of multi-modal wearables emerges from integration. Combined signals reveal patterns invisible to any single modality.
Infection Prediction: The Multi-Modal Signature
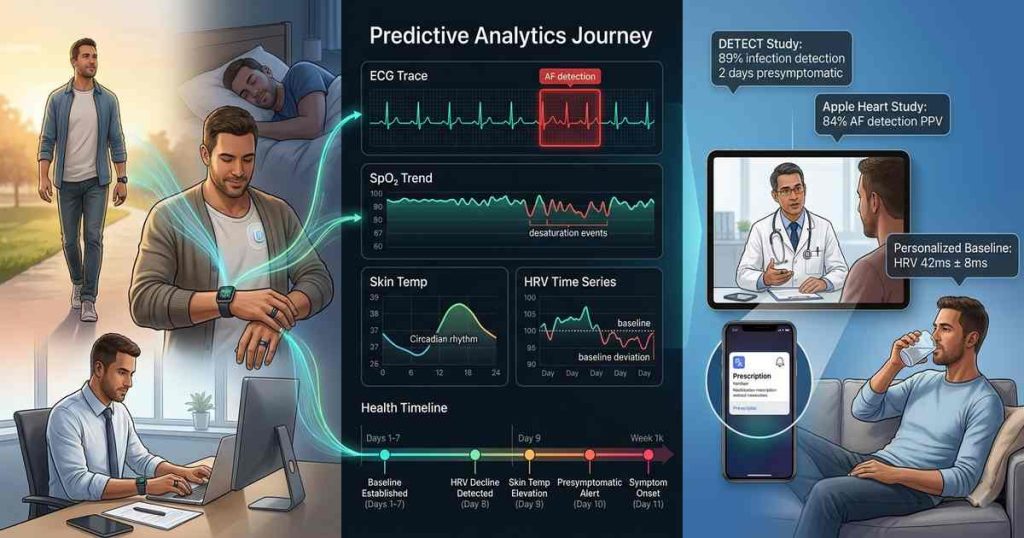
During respiratory infections, the body responds across multiple physiological systems before symptoms appear. Research from the Scripps Research Institute’s DETECT study, which enrolled over 30,000 participants using various wearables, identified a characteristic multi-modal signature of presymptomatic infection:
- HRV decline: Begins 2-4 days before symptom onset (parasympathetic withdrawal)
- Resting heart rate elevation: Increases 1-3 days before symptoms (sympathetic activation)
- Skin temperature elevation: Increases 1-2 days before symptoms (inflammatory response)
- SpO₂ decline: Often begins with or after symptoms (pulmonary involvement)
When these signals are integrated, predictive algorithms can identify infection with 80-90% sensitivity days before the user perceives symptoms. This early warning enables proactive isolation, testing, and early intervention—particularly valuable for immunocompromised individuals, healthcare workers, and during infectious disease outbreaks.
Cardiovascular Risk Assessment
Cardiovascular disease risk assessment traditionally relies on episodic measurements in clinical settings. Multi-modal wearables offer continuous assessment across multiple domains:
ECG: Detects AF episodes (often asymptomatic) that increase stroke risk 5-fold
HRV: Low HRV predicts cardiovascular mortality independently of other risk factors
Resting heart rate: Sustained elevation predicts increased cardiovascular risk
SpO₂: Nocturnal desaturation indicates sleep apnea, a major cardiovascular risk factor
Activity patterns: Declining step count and activity intensity correlate with functional decline
When integrated, these signals generate a continuous cardiovascular risk score that can prompt intervention before acute events. The potential for early detection of developing hypertension—through combinations of resting heart rate, HRV, and activity patterns—is particularly promising.
Sleep Architecture Assessment
Consumer wearables have evolved from crude sleep duration estimates to multi-modal sleep staging:
- Heart rate and HRV: Distinguish REM from non-REM sleep
- Movement (accelerometer): Identifies wake episodes and movement disorders
- SpO₂: Detects apnea-related desaturations
- Skin temperature: Tracks circadian phase and sleep depth
- ECG-derived respiration: Assesses respiratory patterns during sleep
Multi-modal sleep staging now approaches the accuracy of polysomnography (laboratory sleep studies) for basic sleep architecture, though clinical sleep disorders still require formal testing. For individuals optimizing sleep, multi-modal wearables provide actionable insights: when to adjust bedtime, whether recovery sleep after travel is adequate, and how alcohol, caffeine, and exercise affect sleep quality.
Menstrual Cycle and Fertility Tracking
Skin temperature combined with HRV and resting heart rate enables sophisticated cycle tracking:
- Skin temperature: Detects post-ovulatory temperature rise with high precision
- HRV and resting heart rate: Track luteal phase changes and may indicate pregnancy
- ECG: Potential for detecting cycle-related cardiac changes
These signals enable fertility window prediction and cycle phase identification without manual logging, making multi-modal wearables valuable for both conception and cycle-related symptom management.
Data Integration: From Raw Signals to Predictive Analytics
The transformation of raw sensor data into predictive health insights requires sophisticated processing pipelines.
Signal Quality Assessment
The first challenge is distinguishing physiological signal from noise. Wearable sensors on the wrist face constant motion artifacts—arm movement, muscle tension, and environmental interference. Multi-modal systems use cross-sensor validation: if the accelerometer detects movement, the ECG signal may be flagged as unreliable; if skin temperature changes rapidly, it may reflect environmental temperature rather than physiological change.
Machine learning models trained on labeled data (clean vs. noisy signals) can assess signal quality in real-time, discarding unreliable data while preserving clinically valuable information.
Feature Extraction
From cleaned signals, algorithms extract features that correlate with physiological states:
ECG features: Heart rate, RR intervals, QRS duration, QT interval, AF probability
HRV features: Time-domain (SDNN, RMSSD), frequency-domain (LF, HF, LF/HF ratio)
SpO₂ features: Baseline saturation, desaturation events, oxygen desaturation index
Skin temperature features: Baseline, circadian phase, deviation from baseline
Accelerometer features: Activity intensity, sleep/wake classification, gait metrics
Personalization and Baselines
Multi-modal wearables excel because they personalize to each user. Rather than applying population thresholds (“heart rate >100 bpm is tachycardia”), these systems learn each individual’s normal ranges across all modalities.
A user’s normal HRV might be 40 ms; another’s might be 80 ms. The clinically relevant signal is not the absolute value but the deviation from personal baseline. For infection detection, a 20% HRV decline from baseline may be significant even if absolute HRV remains within “normal” population range.
Personalization requires establishing baselines across circadian cycles, activity levels, and environmental conditions. Modern wearables typically require 7-14 days of continuous monitoring to establish stable baselines.
Multi-Modal Fusion
The core predictive analytics challenge is fusing signals that operate on different timescales and represent different physiological systems. Several approaches dominate:
Feature-level fusion: Extract features from each modality, concatenate into feature vectors, and train models on combined features. This approach is straightforward but may miss cross-modal interactions.
Model-level fusion: Train separate models on each modality, then combine predictions (e.g., weighted averaging, stacking). This approach preserves interpretability but may not capture synergistic interactions.
Deep learning fusion: End-to-end deep neural networks that learn to integrate raw or minimally processed signals from all modalities. Transformer architectures, originally developed for natural language processing, have shown particular promise for multi-modal time series fusion, learning cross-modal attention patterns that identify which signals are most predictive at which times.
Graph neural networks: Emerging approaches model physiological systems as interconnected networks, with each sensor modality representing a node. Graph neural networks learn how perturbations in one system propagate to others, potentially enabling prediction of systemic effects from localized signals.
Predictive Algorithms: From Detection to Forecasting
Multi-modal wearable analytics span three predictive horizons:
Real-Time Detection (Seconds to Minutes)
Applications: AF detection during active monitoring, fall detection, acute hypoxemia alerts.
These algorithms prioritize low latency and high sensitivity. Simple models (thresholds, decision trees) may outperform complex models when interpretability and speed are paramount. For AF detection, convolutional neural networks analyzing 30-second ECG segments achieve sensitivity >95% with specificity >98%.
Short-Term Prediction (Hours to Days)
Applications: Presymptomatic infection detection, migraine prediction, seizure forecasting.
These algorithms identify early warning signs that precede clinical events. For infection detection, models integrating HRV, resting heart rate, and skin temperature can predict symptom onset 1-3 days in advance. For migraine prediction, changes in HRV and activity patterns may precede attacks by hours, enabling preemptive medication.
Long-Term Trend Analysis (Weeks to Years)
Applications: Cardiovascular risk assessment, hypertension development, fitness trajectory, aging and frailty assessment.
These algorithms focus on gradual changes across weeks or months rather than acute events. For cardiovascular risk, sustained declines in HRV, increases in resting heart rate, and decreases in activity levels together predict increased event risk over months to years.
Clinical Validation: From Consumer Devices to Medical Tools
The transition from consumer wellness tracking to medical-grade monitoring requires rigorous clinical validation.
Validation Standards
Medical validation requires demonstration that wearable measurements meet accuracy standards:
ECG: ANSI/AAMI EC57 standards for arrhythmia detection algorithms
SpO₂: ISO 80601-2-61 requires accuracy within ±3-4% for medical pulse oximeters
Heart rate: Accuracy within ±5 bpm during motion is typical
Temperature: Clinical thermometers require ±0.1°C accuracy; wrist-based temperature has different reference standards
Consumer devices rarely achieve medical-grade accuracy across all conditions, but they increasingly approach it in controlled settings. The Apple Watch Series 8, for example, demonstrates ECG accuracy comparable to single-lead medical devices for AF detection, and its temperature sensor detects deviations of 0.1°C—sufficient for ovulation tracking though not clinical fever assessment.
Clinical Evidence
Several large studies have established the clinical utility of multi-modal wearables:
Apple Heart Study (2019): 419,297 participants; 0.5% received irregular pulse notifications; of those, 84% had AF on subsequent ECG patch monitoring. Demonstrated that consumer wearables can effectively screen for undiagnosed AF.
DETECT Study (2020-2023): 30,000+ participants; demonstrated that multi-modal signals (HRV, heart rate, activity, temperature) could detect COVID-19 and other respiratory infections with 80-90% sensitivity days before symptom onset.
Fitbit Heart Study (2022): 455,699 participants; algorithm detected previously undiagnosed AF with 98% positive predictive value when confirmed by ECG patch.
Scripps Digital Medicine Initiative: Ongoing validation of multi-modal algorithms for cardiovascular risk prediction, showing that wearable data improves risk prediction beyond traditional clinical factors.
Regulatory Pathway
Several multi-modal wearables have achieved FDA clearance for specific indications:
- Apple Watch: AF detection (cleared), ECG (cleared)
- Fitbit: AF detection (cleared)
- Samsung Galaxy Watch: AF detection (cleared), blood pressure (cleared, region-dependent)
- Withings ScanWatch: AF detection, ECG (cleared)
No consumer wearable currently has FDA clearance for infection prediction, cardiovascular risk assessment, or sleep apnea diagnosis—these remain investigational. However, many companies are pursuing regulatory clearance for expanded indications.
Computational Challenges: Processing at Scale
Multi-modal wearables generate massive data streams. A typical device collects:
- ECG: 250-500 samples/second
- Accelerometer: 50-100 samples/second (multiple axes)
- SpO₂: 1 sample/second (averaged over multiple readings)
- Temperature: 1 sample/minute
- Total: 50-100 million samples per device per month
For millions of users, data volumes exceed 100 petabytes monthly. Processing requires sophisticated edge-cloud architectures:
Edge processing: Real-time algorithms (AF detection, fall detection) run on-device, minimizing latency and preserving privacy. Modern wearables include dedicated neural processing units (NPUs) for AI inference at milliwatt power levels.
Cloud analytics: Long-term trend analysis, population-level insights, and model retraining occur in the cloud. Federated learning approaches enable model improvement without centralizing sensitive user data.
Privacy preservation: Multi-modal health data is among the most sensitive personal information. On-device processing minimizes data transmission; when cloud analysis is required, differential privacy, homomorphic encryption, and secure enclaves protect user data.
Emerging Frontiers
Continuous Blood Pressure
Optical sensors combined with machine learning are enabling cuffless blood pressure estimation. Multiple companies (Samsung, Aktiia, Omron) have introduced wearable blood pressure monitors, though accuracy varies. Multi-modal integration (photoplethysmography + ECG + accelerometer) improves accuracy by accounting for factors affecting pulse wave velocity.
Blood Glucose Monitoring
Non-invasive glucose monitoring remains the “holy grail” of wearables. Current approaches—spectroscopy, optical, and thermal—have not achieved accuracy comparable to continuous glucose monitors (CGMs). However, multi-modal integration combining optical signals, skin temperature, and heart rate may eventually enable accurate enough glucose estimation for diabetes management.
Respiratory Rate
Respiratory rate is a sensitive indicator of illness, yet underutilized in consumer wearables. Multi-modal devices can derive respiratory rate from ECG (R-wave amplitude modulation), accelerometer (chest movement), or photoplethysmography (pulse amplitude variation). Integration across modalities improves accuracy during movement.
Hydration and Electrolyte Balance
Changes in blood volume affect pulse wave characteristics. Multi-modal sensors may eventually estimate hydration status and electrolyte balance—valuable for athletes, workers in hot environments, and patients with heart failure or kidney disease.
The Path Forward: From Reactive to Proactive Health
The ultimate promise of multi-modal health wearables is a shift from reactive to proactive healthcare. Instead of waiting for symptoms to prompt medical visits, continuous monitoring enables:
Early intervention: Treating infections in presymptomatic stages reduces severity and transmission.
Risk stratification: Identifying individuals at highest risk for cardiovascular events enables targeted prevention.
Treatment optimization: Monitoring response to medications enables dose adjustment before side effects become intolerable.
Aging in place: Multi-modal monitoring can detect early signs of functional decline, enabling interventions that maintain independence.
The technology is largely ready. The challenges ahead are less about sensors and algorithms than about integration into healthcare systems, regulatory approval, reimbursement models, and, most fundamentally, ensuring equitable access to the health benefits these devices can provide.
Conclusion
Multi-modal health wearables represent a fundamental advance in personal health monitoring. By integrating ECG, SpO₂, skin temperature, and HRV—and learning what normal means for each individual—these systems can detect emerging illness, track chronic disease, and provide actionable insights that episodic clinical measurements cannot.
The evidence base is growing. Large studies have validated AF detection, infection prediction, and sleep staging. Regulatory approvals are expanding. And the technology continues to improve, with better sensors, more sophisticated algorithms, and deeper integration with healthcare systems.
The transition from wellness tracking to medical monitoring is well underway. The fourth generation of wearables is not just telling us how many steps we took—it is telling us, with increasing accuracy, what is happening inside our bodies, what might happen next, and what we can do about it. For millions of people, that information will be the difference between early intervention and advanced disease, between hospital admission and home recovery, between knowing and not knowing.
The sensors are on our wrists. The analytics are in our devices. The future of proactive, predictive, personalized health is already here.