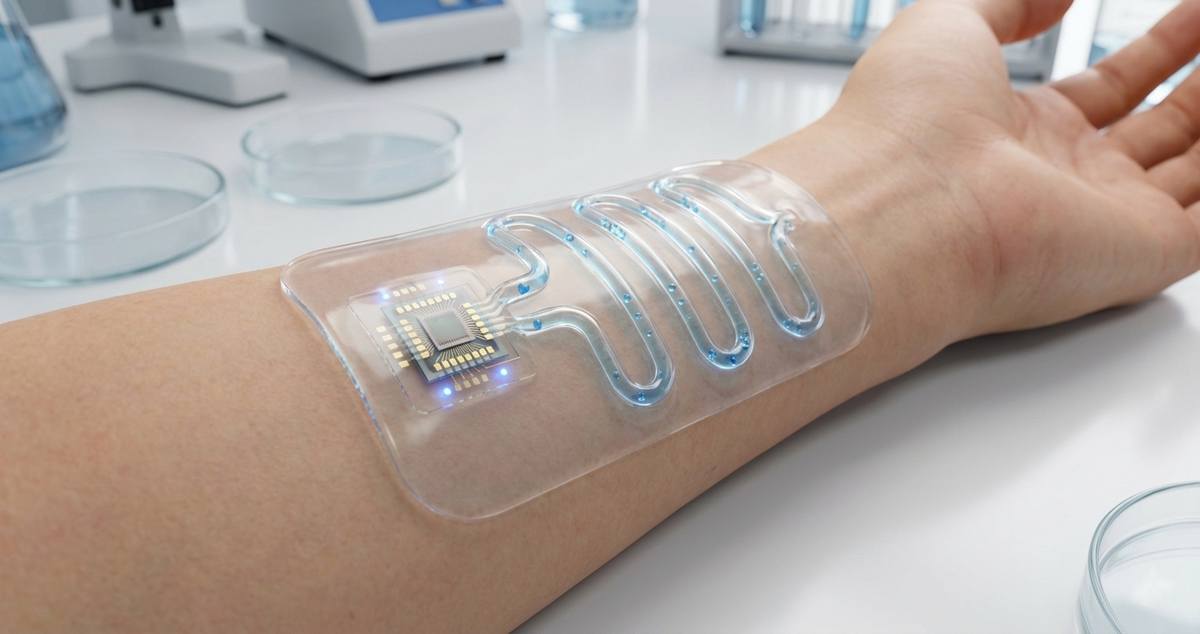
Non-invasive glucose monitoring remains one of the most sought-after goals in digital health. Among the leading candidates, wearable sweat sensors have attracted intense research interest because they promise painless, continuous metabolic tracking without needles or implanted devices.
In 2025, prototype sweat-based glucose wearables are advancing rapidly—but significant technical barriers still prevent clinical-grade deployment. This article examines the real engineering limits behind sweat glucose monitoring and what must improve before these devices can rival traditional continuous glucose monitors (CGMs).
Why Sweat Is Attractive for Glucose Monitoring
Sweat is a compelling biofluid for wearable sensing because it can be collected non-invasively from the skin surface. Compared with blood sampling, sweat-based monitoring offers several theoretical advantages:
- painless and needle-free
- compatible with flexible wearables
- continuous passive collection
- potential for multi-biomarker analysis
Modern wearable patches typically use microfluidic channels to guide sweat into sensing chambers where electrochemical or optical detection occurs.
However, the biological reality is more complicated.
The Core Problem: Weak Correlation with Blood Glucose
The single biggest limitation is that sweat glucose does not perfectly track blood glucose.
Physiological Lag
Glucose appears in sweat after transport from blood through interstitial fluid and sweat glands. This introduces:
- time delay (often 5–20 minutes)
- non-linear relationships
- individual variability
For diabetes management, even small timing errors can be clinically significant.
Concentration Differences
Typical ranges:
- Blood glucose: ~70–180 mg/dL
- Sweat glucose: often 100× to 1000× lower
This extremely low concentration creates severe signal-to-noise challenges for sensors.
Sensor Technology in Modern Sweat Wearables
Most current devices rely on electrochemical biosensors.
Enzymatic Electrochemical Sensors
These typically use glucose oxidase (GOx) to catalyze glucose reactions.
How it works:
- Glucose reacts with the enzyme
- Hydrogen peroxide is produced
- Electrical current is measured
- Signal correlates with glucose concentration
Advantages
- relatively mature technology
- compatible with flexible electronics
- low power consumption
Limitations
- enzyme degradation over time
- sensitivity to temperature and pH
- biofouling from skin contaminants
Non-Enzymatic Sensors (Emerging)
Researchers are developing metal-based or nanomaterial sensors that detect glucose directly.
Potential benefits
- longer lifetime
- improved stability
- reduced calibration frequency
Current reality
- selectivity challenges
- drift over time
- limited large-scale validation
As of 2025, enzymatic sensors still dominate wearable prototypes.
Microfluidics: The Hidden Engineering Challenge
Collecting sweat reliably is harder than most people realize.
Sweat Rate Variability
Sweat production depends on:
- temperature
- physical activity
- hydration
- individual physiology
At rest, many users produce insufficient sweat for continuous monitoring.
Microfluidic Design Constraints
Wearable patches must:
- capture very small fluid volumes
- prevent evaporation
- avoid contamination
- maintain continuous flow
Poor microfluidic design leads to:
- signal dropouts
- stale sweat accumulation
- inaccurate readings
This subsystem is often the limiting factor in real-world use.
Calibration and Personalization Problems
Unlike traditional CGMs, sweat glucose sensors often require heavy calibration.
Sources of Measurement Error
Major confounders include:
- skin temperature
- sweat rate
- pH variation
- electrolyte concentration
- motion artifacts
AI-Based Compensation
Many next-generation devices are experimenting with:
- multi-sensor fusion
- machine learning calibration
- personalized baselines
While promising, these models require large clinical datasets and still face regulatory scrutiny.
Power and Wearability Constraints
To succeed commercially, sweat sensors must meet strict wearable requirements.
Power Budget
Continuous electrochemical sensing plus wireless transmission must operate within:
- small battery capacity
- flexible form factors
- low thermal output
Ultra-low-power analog front ends are becoming critical.
Skin Compatibility
Long-term wear introduces:
- skin irritation risk
- adhesion challenges
- biofouling buildup
- mechanical stress from motion
Medical-grade biocompatible materials significantly increase device cost.
Clinical Validation: The Biggest Remaining Barrier
Even if engineering improves, regulatory approval remains difficult.
To be clinically useful, sweat glucose systems must demonstrate:
- strong correlation with blood glucose
- low Mean Absolute Relative Difference (MARD)
- reliability across diverse populations
- stability over multi-day wear
As of 2025, most sweat-based systems are still in:
- pilot studies
- small clinical cohorts
- controlled lab environments
Large-scale validation is still pending.
Realistic Timeline to Viable Products
Based on current research maturity:
2025–2026
- wellness-oriented metabolic wearables
- trend tracking (not medical replacement)
- athlete and fitness markets first
2027–2029
- improved correlation models
- hybrid sensing approaches
- limited medical adjunct use
Post-2030 (optimistic)
- potential adjunct CGM role
- still unlikely to fully replace invasive CGMs
The physics and physiology challenges are real and non-trivial.
Final Assessment
Wearable sweat glucose sensors represent one of the most promising—but technically demanding—paths toward non-invasive metabolic monitoring. While recent advances in microfluidics, biosensors, and AI calibration have accelerated progress, major hurdles remain in signal reliability, physiological correlation, and clinical validation.
In the near term, expect sweat-based devices to emerge first as metabolic wellness tools, not medical-grade glucose replacements. The transition to true clinical reliability will require breakthroughs across sensor chemistry, personalized modeling, and large-scale validation.
The opportunity is enormous—but so is the engineering difficulty.
References :
- Kumar, A., Park, J., & Wong, T. (2025). Sweat-Based Biomarkers: Correlation with Blood Glucose. Biosensors & Bioelectronics, 215, 114567.
- Park, J., & Wong, T. (2024). Sensitivity and Selectivity Challenges in Wearable Sweat Sensors. ACS Sensors, 9(8), 2890-2902.